Dizzy? Might be Vestibular Neuritis!
Article by Shayne Alyward
Have you experienced a short, sudden spell of spinning vertigo and imbalance following a recent illness? Do you experience ongoing balance and dizziness? Vestibular Neuritis may be the culprit.

Vestibular Neuritis is a sudden onset of dizziness, vertigo (the sensation of the environment spinning), nystagmus (rapid involuntary eye movements), trouble tracking or focusing on objects, and often nausea and vomiting (1,2,3). Symptoms in most cases will occur soon after a viral infection and typically affect one side of the vestibular system. However, in rare cases due to dormancy and the virus’s ability to remain hidden within the body, symptoms could appear several weeks or months later (1, 2, 3).
There are 2 main phases: acute and chronic. The acute phase occurs as a single significant event that lasts for a couple of days to weeks. Symptoms will persist at rest and worsen with movement. During the chronic phase, imbalance and dizziness may persist for weeks or months (3).

What causes Vestibular Neuritis?
The exact cause of Vestibular Neuritis remains uncertain. However, experts believe it is linked to a viral infection of the vestibulocochlear nerve (8th cranial nerve). Herpes Simplex and Herpes Zoster virus are the most common viral infections linked to Vestibular Neuritis, but several others, such as mumps, measles, hepatitis, polio, Epstein-Barre, and influenza have also been associated (1, 2, 3).
Anatomy
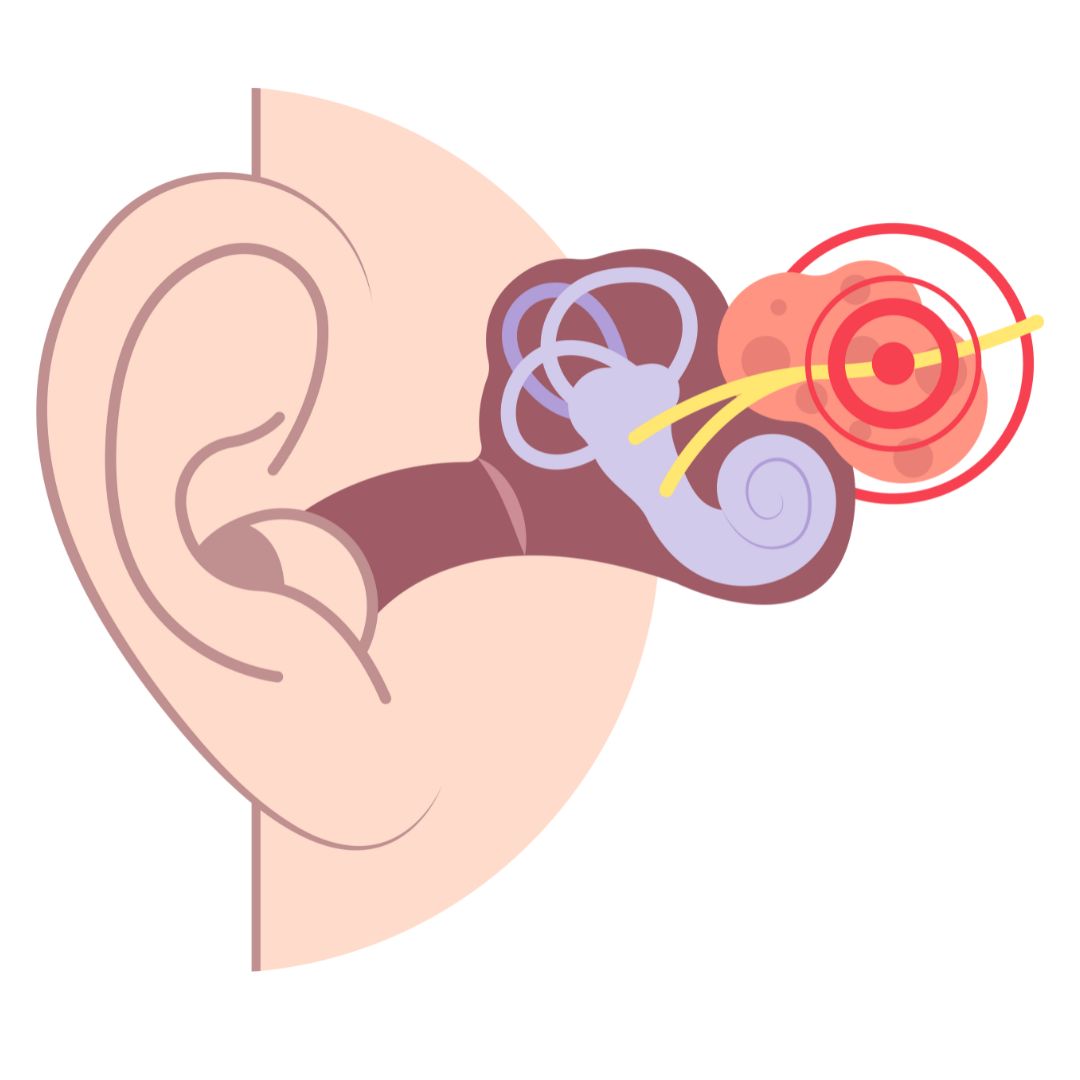
The inner ear contains the vestibular labyrinth which includes three semi circular canals, specialized structures, fluid, and small crystals (Otoliths), that detect head movement and position and are essential in maintaining head position, orientation and posture. The information provided by the vestibular system is relayed to the brain via the Vestibulocochlear nerve. The interruption in nerve transmission causes a disconnect between our eyes and our head movement ultimately leading to dizziness and balance deficits (1, 3).
Diagnosis
An accurate subjective history is key for diagnosis. Key bits of information include onset, duration, triggers, positional changes and whether hearing is affected. Past medical history should be reviewed to rule out risk factors. Due to symptom similarity, it is important to rule out more severe neurological conditions (1, 2, 3). The clinical examination includes visual tests, balance tests, as well as head positional tests for vertigo (1, 3).
Treatment
Treatment during the acute phase focuses on symptom relief and ensuring patient comfort. Although symptoms tend to resolve on their own in a few days or weeks without intervention, doctors can prescribe medications to help reduce nausea, dizziness and vertigo (1, 3).
After the acute phase, treatment becomes a bit more provocative and is aimed at helping the brain adapt, or compensate, for abnormal input from half of the vestibular system. While most people will recover fully, some may continue to experience chronic dizziness and imbalance requiring Vestibular Rehabilitation, usually directed by a specially trained physiotherapist. Retraining includes static and dynamic balance exercises, gaze stabilization, visual tracking, habituation, compensation, and gait challenges. It is important to understand that vestibular rehabilitation is a gradual process often taking weeks, months or even years (1, 3).
References
- Balance and Dizziness Canada. (2019). Vestibular Neuritis. Retrieved January 17, 2025, from https://balanceanddizziness.org/disorders/vestibular-disorders/vestibular-neuritis/
- Strupp, M., Bisdorff, A., Furman, J., Hornibrook, J., Jahn, K., Maire, R., ... & Magnusson, M. (2022). Acute unilateral vestibulopathy/vestibular neuritis: Diagnostic criteria. Journal of Vestibular Research, 32(5), 389-406.
- Shupert, C. L. (2018). Vestibular Neuritis and Labyrinthititis.
You May Also Like...
-
 ArticleView Post
ArticleView PostInjectable Therapy (Part 2 of 2): Hyaluronic Acid, Perineural Injections, & Trigger Point Injections
The more commonly discussed injectable therapies are mentioned in Part 1 of this article. Part 2 of this article contains additional injectable therapies that have been found to be beneficial for chronic pain.
-
 ArticleView Post
ArticleView PostStrengthening the Intrinsic Muscles of the Foot
Learn about the importance of exercising and strengthening your foot's intrinsic muscles – as well as what they are!
-
 ArticleView Post
ArticleView PostOffice Ergonomics & Improving Your Workspace
Ergonomics is the science of designing the workplace environment to fit the worker. By adjusting the workstation to the individual needs of the worker, many common injuries can be prevented.